Medical Malpractice
in Sarasota
Your Guide to Doctor Errors, Misdiagnosis, and Medical Justice
Hospitals and clinics in Sarasota, including Sarasota Memorial and other local facilities, are dedicated to providing care, but mistakes can still occur. Misdiagnoses, surgical errors, or medication issues may leave patients facing additional challenges. Florida law outlines certain protections and procedures in these situations, but navigating them can be complex. This guide is intended to help Sarasota residents understand the risks associated with medical care and learn about available community and support resources. For medical treatment or legal concerns, individuals should seek guidance directly from licensed healthcare providers or attorneys.
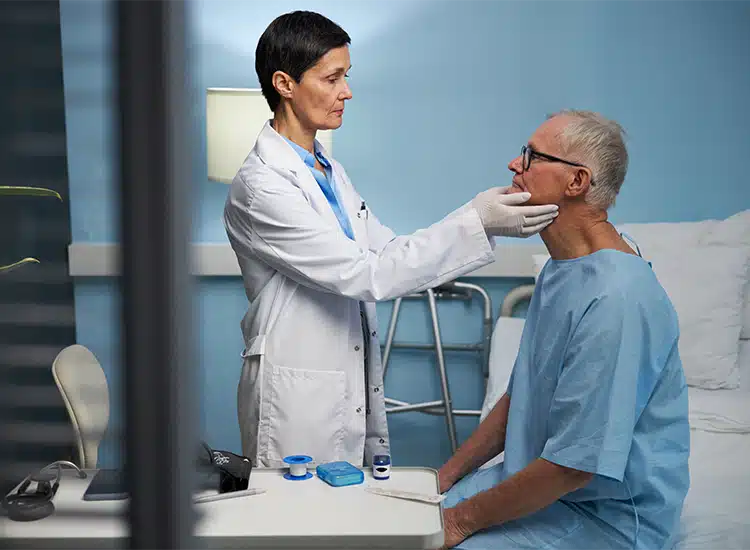
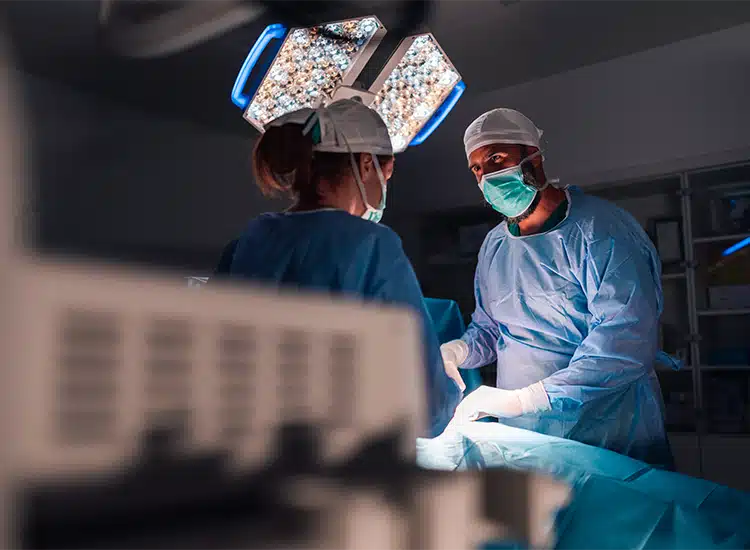
Understanding Medical Malpractice
Medical malpractice falls under personal injury law, requiring proof a healthcare provider’s negligence caused harm (Florida Statute 766.102). Sarasota’s aging population and medical tourism raise the stakes.
Residents can stay proactive by asking questions about their care and reporting concerns to authorities. Resources like the Florida Agency for Health Care Administration provide information on healthcare standards, while the Sarasota Memorial Hospital offers medical care for injuries. The Sarasota County Bar Association can assist in finding licensed attorneys for legal guidance.
FEDERAL FACTS ABOUT MEDICAL MALPRACTICE
**FACT ONE: STATUTE OF LIMITATIONS OVERVIEW** – In the United States, the statute of limitations for medical malpractice claims generally ranges from one to three years from the date of injury or discovery, but this varies by state and can include discovery rules allowing additional time if the harm wasn’t immediately apparent, emphasizing the need to act swiftly to avoid barred claims.
**FACT TWO: STATE-BY-STATE VARIATIONS** – As of 2025, states like Alabama, Alaska, Arizona, and Arkansas impose a two-year limit from the injury date, while California extends to three years from injury or one year from discovery; New York allows 30 months from malpractice or end of treatment, and Connecticut caps at three years absolute from the act, with recent reforms in New York potentially adjusting timelines for certain claims.
**FACT THREE: KEY SIGN FOR PATIENTS – UNEXPECTED COMPLICATIONS** – Patients should watch for unanticipated setbacks post-treatment, such as infections, excessive bleeding, or worsening symptoms that deviate from informed recovery expectations, as these often signal a breach in standard care protocols.
**FACT FOUR: ANOTHER RED FLAG – MISSED OR WRONG DIAGNOSIS** – A common indicator arises when symptoms are ignored, tests are skipped, or an incorrect diagnosis leads to delayed or improper treatment, potentially causing further harm like untreated progression of conditions such as cancer or infections.
**FACT FIVE: PREPARING STEP ONE – SECURE MEDICAL RECORDS** – To build a strong case, immediately obtain all relevant medical records, including charts, test results, x-rays, billing statements, and correspondence, as these form the evidentiary backbone proving deviation from care standards and causation of damages.
**FACT SIX: ESSENTIAL PREP – CONSULT A SPECIALIZED ATTORNEY** – Schedule free initial consultations with attorneys experienced in medical malpractice, providing a timeline of events, provider details, and records to assess viability, as most firms work on contingency without upfront fees.
**FACT SEVEN: GATHER EXPERT TESTIMONY EARLY** – Preparation includes identifying and retaining medical experts to review records and opine on whether the care fell below accepted standards, a critical element required in nearly all states to establish the breach of duty.
**FACT EIGHT: SUING DOCTORS – DIRECT NEGLIGENCE FOCUS** – When suing an individual doctor, claims center on personal failures like surgical errors, prescription mistakes, or inadequate informed consent, holding the physician accountable for deviating from the professional standard of care expected in similar circumstances.
**FACT NINE: SUING HOSPITALS – VICARIOUS AND DIRECT LIABILITY** – Hospitals face suits under vicarious liability for employees’ negligence or direct liability for institutional failures like understaffing, faulty equipment, or failure to supervise contractors, even if the doctor is independent, provided the hospital didn’t disclose that status.
**FACT TEN: WHEN TO SUE BOTH – OVERLAPPING CLAIMS** – In many cases, both doctor and hospital can be targeted simultaneously if the negligence involves coordinated care failures, such as miscommunication between staff leading to medication errors, allowing plaintiffs to pursue full compensation from multiple deep-pocketed defendants.
Common Injuries and Florida Law
Misdiagnosis
The Injury
Missing cancer or a heart issue like at a local clinic delays treatment.
The Law
Prove the doctor breached standard care and caused harm expert testimony needed.
Sarasota Case
A 2022 misdiagnosis settled for $750K delay worsened prognosis.

Surgical Errors

The Injury
Wrong-site surgery or left instruments like at Sarasota Memorial cause pain or infection.
The Law
Negligence claims cover damages; caps at $500K-$1M for pain.
Stat
Florida sees hundreds of surgical error cases yearly.
Medication Mistakes
The Injury
Wrong drugs or doses like in a retiree-heavy area can kill.
The Law
Pharmacy or doctor liability if standard care fails.

Florida’s Malpractice Rules
Pre-Suit
Time Limit
2 years, extendable to 4 with discovery (Florida Statute 95.11).
Caps
$500K non-economic damages, $1M for catastrophic cases.
MEDICAL MALPRACTICE CASES OF NOTE IN FLORIDA
Maya Kowalski v. Johns Hopkins All Children’s Hospital – $220 million – 2023 – A 10-year-old girl was wrongfully committed and separated from her mother, leading to emotional distress and the mother’s suicide. The case gained massive fame through the Netflix documentary “Take Care of Maya.”
Allan Navarro v. Tampa University Community Hospital – $216.7 million – 2006 – A former basketball player suffered permanent brain damage after his stroke was misdiagnosed as sinusitis by an unlicensed physician’s assistant, resulting in delayed treatment and coma.
Unnamed Plaintiff v. University of South Florida – $109 million (capped due to sovereign immunity) – 2010 – During ovarian cyst surgery, the surgeon cut the patient’s intestine, causing sepsis, gangrene, and amputation of her hands and feet.
Lubben v. Lopez – $100 million – 2024 – Surgical errors during a procedure, involving unlicensed activity and lack of informed consent, led to severe bodily injury.
Chiaka Stewart v. Tampa General Hospital – $70.8 million – 2025 – A woman suffered blindness, paralysis, and cognitive impairments after being discharged from the ER without proper stroke evaluation, despite clear symptoms.
Miranda Crohan v. University Community Hospital, Inc. – $68.8 million – 2022 – Four physicians’ negligence caused severe brain damage to a patient during treatment.
Unnamed Woman (Paraplegia Case) – $65.3 million settlement – 1997 – Induced labor with Pitocin and epidural complications led to paraplegia and cauda equina syndrome, with no sensation in the legs.
James Sada v. Orlando Health – $45 million – 2025 – Delayed transfer for a heart attack due to hospital prioritization issues resulted in the patient’s death.
Marla Dixon v. North Shore Medical Center (Earl Reese-Thornton Jr. Case) – $33.8 million – 2013 – Birth injuries causing brain damage to a newborn after the doctor delayed a C-section, resumed excessive medication, and left for personal calls.
Estate of Sasso v. Cleveland Clinic Florida – $31.9 million – 2024 – Wrongful death due to delayed treatment and failure to diagnose or monitor the patient’s condition adequately.
What to Do After Malpractice
Get Second Opinion
Confirm any potential harm with a second opinion, and keep updated records to support ongoing care and documentation.
Gather Records
Keep organized copies of medical records, bills, and other related documents to track your care and expenses.
Seek Professional Support
Residents seeking legal guidance should consult directly with licensed local attorneys.
MEDICAL MALPRACTICE MYTHS
Medical malpractice can be a confusing and intimidating topic for patients. Misconceptions often prevent people from seeking justice or understanding their rights after a medical error. Below, I’ve debunked some of the most common myths based on reliable legal and medical sources. Knowing these facts can empower you to make informed decisions if you suspect negligence. Remember, if you’ve been harmed, consulting a qualified attorney is key—they can evaluate your case without upfront costs in many instances.
Myth: Most medical malpractice claims are frivolous lawsuits filed by greedy patients. Fact: In reality, only a small fraction of medical errors lead to claims, and these suits are far from frivolous. They often stem from genuine harm, and malpractice costs make up less than 3% of U.S. healthcare spending. This myth is perpetuated by insurance companies, but studies show more malpractice occurs than is ever litigated. Patients should know that filing a claim holds providers accountable and can improve overall care standards.
Myth: If a doctor makes any mistake, it’s automatically medical malpractice. Fact: Not every error qualifies as malpractice. You must prove four key elements: the provider owed you a duty of care, they breached the standard of care (what a reasonable professional would do), the breach caused your injury, and you suffered damages. Simple human errors without negligence don’t count. As a patient, document everything—medical records, symptoms, and communications—to build a strong case if needed.
Myth: Signing a consent form means you can’t sue for malpractice. Fact: Consent forms acknowledge known risks of a procedure but don’t protect against negligence, like failing to meet care standards or making avoidable errors. You can still sue if harm results from substandard care. Patients should read forms carefully and ask questions, but know your rights aren’t fully waived.
Myth: Medical malpractice lawsuits are an easy way to get rich quick. Fact: These cases are complex, time-consuming, and hard to win, often taking years with expert testimony required. Awards are meant to cover real losses like medical bills, lost wages, and pain—not windfalls. The median payout is around $400,000, and many cases settle for less. For patients, focus on recovery first; lawsuits are about fairness, not fortune.
Myth: Only doctors can be sued for medical malpractice. Fact: Nurses, pharmacists, anesthesiologists, hospitals, and other providers can all be liable if their negligence causes harm. Hospitals may be responsible for their employees’ actions under vicarious liability. Patients should identify all parties involved in their care when considering a claim.
Myth: You can file a malpractice lawsuit at any time after an injury. Fact: Statutes of limitations vary by state (e.g., 2-4 years from the injury or discovery), and missing the deadline can bar your claim forever. Some exceptions exist, like for minors or delayed discovery of harm. Act promptly—patients should consult a lawyer soon after suspecting malpractice to preserve evidence.
Myth: Malpractice suits drive up healthcare costs significantly. Fact: This is overstated; malpractice accounts for a tiny portion of costs. Main drivers are administrative expenses, drug prices, and inefficiencies. Suits actually promote safer practices by encouraging accountability. Patients benefit from this system as it incentivizes better care overall.
Myth: Only surgical errors qualify as medical malpractice. Fact: Malpractice includes misdiagnosis, medication errors, birth injuries, failure to treat, anesthesia mistakes, and more. Any deviation from standard care that causes harm can be grounds. Patients should be aware that non-surgical issues, like ER negligence, are common claims.
Myth: Filing a claim will lead to retaliation from healthcare providers. Fact: Providers are legally and ethically bound to continue care without discrimination. Retaliation is illegal, and you can report it if it occurs. Don’t let fear stop you—patients have protections.
Myth: Most cases go to trial and are decided by biased juries. Fact: The majority settle out of court through negotiations. Juries aren’t inherently anti-doctor; studies show they’re fair and often side with providers when evidence is weak. For patients, this means quicker resolutions are possible with strong representation.
If you’re dealing with a potential malpractice issue, gather your medical records, note timelines, and seek a free consultation from a specialist attorney. Knowledge dispels fear—stay informed to protect your health and rights.
Mistakes to Avoid
Failing to keep thorough records, such as medical files and expenses, can weaken your ability to track what happened. Missing critical deadlines, such as those set by Florida’s statute of limitations, can limit available options. Staying organized, asking questions, and acting promptly are key steps in avoiding these pitfalls.
Getting Your Recovery
We encourage residents to explore local support options, such as the Sarasota Memorial Hospital for medical care or the Sarasota County Bar Association to find licensed attorneys for legal guidance. For healthcare safety resources, visit the Sarasota County Health Department.
Quick Facts
| Injury | Key Rule |
| Misdiagnosis | Prove delay caused harm. |
| Surgery | Negligence caps at $500K-$1M. |
| Medication | Fault unlocks damages. |
| Time Limit | 2 years, up to 4 with discovery. |
MALPRACTICE FACTS FOR PHYSICIANS
Protecting Physicians: Medical Malpractice Insurance and Things for Doctors to Know
Medical malpractice insurance is essential for physicians to safeguard against the financial and professional risks of lawsuits. It covers claims of negligence or errors in care, helping with legal fees, settlements, and judgments. Doctors should understand the basics of this insurance, how to choose it, and broader strategies to minimize lawsuit risks. This knowledge can reduce stress and promote better practice habits. Always consult with insurance experts or attorneys for personalized advice, as laws vary by state.
What is Medical Malpractice Insurance?
Medical malpractice insurance, also known as professional liability insurance, protects physicians from financial losses due to lawsuits alleging negligence in providing medical services. It typically covers defense costs, settlements, and court judgments up to the policy limits. Without it, a single claim could devastate a doctor’s finances and career. Most states require physicians to carry this insurance, and it’s often provided by employers for hospital-based doctors, but independent practitioners need their own policies.
Types of Malpractice Insurance Policies
There are two main types: claims-made and occurrence. Claims-made policies cover claims reported while the policy is active, requiring “tail” coverage for claims after the policy ends (e.g., upon retirement or switching insurers). Occurrence policies cover incidents that happen during the policy period, even if the claim is filed later—no tail needed. Claims-made is more common and often cheaper initially, but tail coverage can add costs.
How to Choose a Malpractice Insurer
Evaluate carriers based on financial stability, claims-handling reputation, and defense quality—look for A.M. Best ratings of A or higher. Consider using a broker for comparisons, as they can shop multiple options without bias. Ask about policy limits (e.g., $1 million per claim/$3 million aggregate), exclusions, and consent-to-settle clauses, which give you a say in settlements. Direct purchase from carriers might save time but limits options.
Factors Affecting Insurance Costs
Premiums vary by specialty (higher for high-risk fields like surgery), location (states with tort reform have lower rates), and claims history. New doctors might get discounts, but expect rates to rise with experience. Shop around annually and consider group policies through medical associations for better rates.
Importance of Tail and Nose Coverage
If switching from a claims-made policy, get tail coverage for past incidents or “nose” (prior acts) coverage from the new insurer. Without it, you’re exposed to uncovered claims. Employers sometimes provide this when you leave, but confirm in writing.
Beyond Insurance: Asset Protection Strategies
Develop an asset protection plan alongside insurance, such as trusts or retirement accounts, to shield personal assets from judgments exceeding policy limits. This is crucial since lawsuits can target savings, homes, or investments. Consult a financial advisor experienced in physician planning.
Documentation Tips to Avoid Lawsuits
Thorough, accurate records are key—document patient discussions, thought processes, and follow-ups to defend against claims. Avoid alterations, judgmental language, or templates that seem generic. Address notes from nurses or consultants, and ensure timely entries to reduce liability risks.
Communication with Patients
Clear, empathetic communication builds trust and reduces sue risks—explain treatments, risks, and listen to concerns. Obtain informed consent properly, and document it. Positive relationships make patients less likely to litigate even if outcomes are poor.
Risk Management Practices
Stay updated with continuing education, follow evidence-based protocols, and participate in peer reviews. High-risk areas like diagnosis delays (e.g., cancer, strokes) warrant extra caution. Implement office systems for test follow-ups to prevent oversights.
Responding to a Lawsuit
Notify your insurer immediately upon notice—don’t discuss the case without counsel. Avoid self-representation or altering records. Litigation is stressful; seek emotional support to maintain well-being.
Common Pitfalls to Avoid
Don’t assume employer coverage is sufficient for all scenarios, like moonlighting. Miss deadlines for claims reporting, or ignore state statutes of limitations. Over-relying on defensive medicine doesn’t always reduce risks and can increase costs.
If facing potential issues, review your policy, strengthen documentation habits, and consider risk management training. Protecting your practice involves both financial safeguards and proactive care strategies to ensure long-term security.
Looking For Information About Medical Malpractice in Sarasota?
This resource is created to support Southwest Florida residents by providing access to local information, community services, and helpful guidance on issues that impact daily life.
